In 2016, Dr. Shah traveled to Albuquerque with MASS Design Group to visit Dar a Luz, a freestanding birth center that has been operating since 2008. This visit was part of a larger body of work supported by the Robert Wood Johnson Foundation exploring how the layout of a birthing space can affect patient outcomes, and specifically hospital c-section rates. As Neel describes in his most recent OBservation, Dar a Luz is intentionally built around the physical and psychosocial needs of a birthing person opposed to the convenience of physicians and pace of a hospital. Fascinated by his experience, I recently chatted with Abigail Lanin Eaves, a co-founder of Dar a Luz, to learn more. We talked about everything from the selection of art for the birth center to the lack of postpartum support for new parents. Enjoy!

Jocie: Can you start by telling me a little bit about the founding of Dar a Luz, the mission, and what inspired you to start it?

Abigail: Sure. So I learned about birth centers when I was in midwifery school, so in 2000. When I started midwifery school, several of my instructors had practiced in birth centers. And there was a birth center in Albuquerque that had closed down I think in the mid-80s, so it just felt like this was the location to have a birth center. And I knew even at that point that home birth was very well supported in New Mexico. And at the time, I was a postpartum nurse, and I met so many women, especially multips [multiparous – someone who has given birth before] who said they didn’t feel comfortable or safe being at home, but if there was a birth center they would love to have that option. So I was making mental notes of that as a very young nurse, and as a sprouting midwife, and I just knew that was what I needed to do.
Fast forward to 2007, I started developing with Alisa Henning, my original business partner. We worked together for about two and a half years and then she moved away and now she’s been back with us for a year and a half, which is really awesome. So we developed for nearly four years before we opened our doors. It was really important to be a non-profit for me for multiple reasons, but I think health care should be a non-profit venture. And it just feels like pregnant people should have the opportunity to birth where they want and be supported in any environment.
Jocie: What barriers did you come up against in the four years it took to develop the center?
Abigail: Oh gosh, I think the main thing that took a while – well certainly money, financial barriers – but also within the Department of Health, no one could figure out how or whether we should be licensed, so the biggest barrier we came up against was reimbursement for the facility services. But in development, it was hard to know how that was going to play out. I think we actually had a lot of really good support. And even from the Department of Health, they said it’s not illegal to operate and they won’t come and shut us down, we just don’t know if you had a license, where that would be. So it was really time management and money that were the biggest barriers for those four years.
Jocie: Yeah, it sounds like you were really trailblazing and people were like “we don’t know what to do with you.”
Abigail: Yeah pretty much. But at the time there was a freestanding birth center in Taos, New Mexico which is further north that was operated by licensed midwives for about 25 years and was a well known birth center. I think they never really tried very hard to get facility reimbursement and flew under the radar, mostly just billed for their professional services. So the Department of Health knew that they were operating and was never concerned or said that birth centers can’t operate without a license. Instead it was us who pushed to get a license so we could be recognized by Medicaid and all the payers for facility reimbursement.
Jocie: And I’m sure that’s huge for patients and increases the patients you can offer services to. So I would love to hear a bit about the physical design. What were some principles you thought about when you were planning and building the birth center?

Abigail: There were a few things. So Melanie Yanke became my partner in crime at the end of 2010. She had done her masters thesis on the physical space and design. I had done my masters thesis on the feasibility of a birth center. So part of what was really important to me was when I worked in my hospital-based practice, I felt like the physical space could have been any office or any unit. There was so little that celebrated pregnant and birthing people, the art on the walls were landscapes that you could buy at any store. So to me, the artistic part was really big. Melanie came in and thought about the design and how we support birthing people in physiologic labor.
And we spent hours and hours while the space was being renovated putting down blue tape and measuring things out to the inch. For instance, if we have a table this big and it fits here, how many steps does it take to get to the tub, and if we have this big of a tub, and it’s this far from the toilet, etc. We really thought about the placement of every single thing, all the way down to the artwork on the wall and how the space flowed for a woman in labor and how it flows for family members and staff. And sometimes you don’t even know until it happens. Everything is moving and we know that. And I think that’s one of the problems with hospitals. Things are built into the wall and they try to make it look like things aren’t so medicalized, but then they’re stuck with how things flow. And we haven’t had to change our design because it actually works really well and we thought about most of the big things from the beginning, but people come to us not just because it’s a birth center, but because that physical space feels so welcoming and open to them.

Jocie: Yeah, and to have that flexibility to change based on inputs I’m sure just improves the experience. I think hospitals think a lot about the clinician and what’s important to them and their workflow, but you’re able to put the patient in the center. I saw on your website that you have a lot of postpartum support for families. Can you tell us a bit more about that and how you think about that support?
Abigail: So first of all, there are the visits with the midwives. If they deliver with us, we do a home visit – as long as they are within a 30 minute range – in the first 24-36 hours. And the midwives still do all of the home visits. If they deliver at the hospital, we go and do courtesy rounds. After that 24 hour visit, as long as everything looks okay, we see them back at three days. And these are mom/baby visit, so we see the dyad for the first 28 days. A lot of birth centers don’t do newborn care for different reasons. For me and for us, we can’t separate them out, and that’s made a huge difference in our practice and with the mothers feeling supported because they can ask questions about their babies and we’re not saying “well, I can’t really answer that for you”. So there’s the three day visit, and as long as everything seems good, we see them back for a two week visit and then a four week visit, and then the babies are discharged from care and we see the mom back for her six to eight week postpartum visit. We also have lactation services. We have three IBCLCs (International Board Certified Lactation Consultant) on staff and we have 24/7 availability, so if someone needs to come in on a weekend or a holiday for those visits, we don’t shuffle them off to another day because it’s Christmas. If someone has a three day visit, and it’s Christmas, then that’s what we’re doing. And then there’s 24/7 availability for the midwives once they register for care. So we have a fair amount of parents who are depressed or anxious, and the fact that they have a lifeline to us makes a big difference. They know that in crisis or not crisis, they can get to us.
And we also have our support groups which kind of go in and out of favor. I think it’s really hard once you have a baby. We have our weekly breastfeeding support group which is incredibly popular. This is open to all people in the community, not just people who gave birth at the center. And so now our breastfeeding support group is better attended by women from the community who have no other support than our own. So that’s really great. We have a mindful parenting group with our licensed health care worker and her partner. And he leads a mens partner group the opposite months which is getting better attendance too. We’ve tried some other support groups. We tried a birth trauma group, that didn’t go over so well. I think people don’t like the word trauma until they’ve come to the conclusion that they’ve been traumatized. And we have a postpartum support group that happens every month as well with Kimberlee, our mental health care worker. And we just started a Pappy hour also for men and they meet at local breweries and support each other and that’s taken off again. And again it’s all free, open to all community members.
Jocie: That’s incredible. And the medical support that you describe postpartum – three or four visits for mom and baby before six weeks. That’s amazing.

Abigail: Yeah, it’s really helpful. And we get these babies sometimes that are not feeding well. I’m seeing lots of tongue and lip ties, lots of different things. Sometimes we see them ten or twelve times in six weeks, and I can’t imagine what else parents are doing in these situations. I guess they’re just going at it alone and giving up and don’t have support. The people we serve tend to have higher education and are more affluent, and they’re still really struggling, so I worry about those we aren’t reaching right now, partially because of our location, partially because it’s hard to reach them for different reasons. But I worry about the state of motherhood in this country.
Jocie: Absolutely and in that vein, are there any practices in the birth center that you think could be implemented in a hospital and improve outcomes and experiences?
Abigail: Yes. I think we’re certainly failing mothers in the postpartum period. When I had my first son, who’s going to be 23 years old, I had a two week and a six week visit and I did have a home visit from a nurse, I remember that. And I think now most birthing people only get a six week postpartum visit and that’s just an absolute failure. Certified nurse midwives (CNMs) – and even licensed midwives, even though they’re not in the hospital practice – we all have within our scope newborn care, and I think it’s such a disservice to split mom and babies. Babies have to go to a pediatrician and mom maybe gets a postpartum visit or two, and I think CNMs can do more in hospital practice. I don’t know if they would all agree with me on that, but that would shift outcomes, and just having access to a provider more often. At least three visits in the first six weeks, especially for first time moms. I think those are the main things that can be shifted. Unfortunately hospital based practice is really based on RVUs (Relative Value Units) and how many patients you can see. Birthing people need hour long visits – a 15 minute visit isn’t going to cut it.
Jocie: Yeah and at that point it’s about the payment systems and incentives for providers and it’s so wrapped up in this huge system.
Abigail: Exactly.
Jocie: Is there anything else about the birth center that you’d like to share?
Abigail: I could talk about the birth center for days. I would really like to include what an amazing group of women I have working for and with me. And birth centers cannot be successful without the people who work there. It’s not just the vision of one person. My staff has been the most incredible to work with – they have followed me into the trenches and back out and back in. And I think one of the unfortunate things about birth center practice, that people who work there – nurses and midwives – know what a huge commitment it is. It’s hard to get people to commit to that kind of practice. I would love to see more midwives really open back up to giving that kind of family centered care because we really need it in the country
Jocie: It’s really a lifestyle. I think about that a lot – how in this country we think of work and home as so separate. And there are so many professions – it sounds like working at a birth center is one of them – where we need to think about life and careers holistically, and I think we’re disincentivized to think that way based on social and family support in this country.
Abigail: Yes and more and more we’re wanting to work less and make more and willing to give up the heart of what we do. I had a great job at the hospital I was working at. I worked per diem, I made my own schedule, I made good money, but I had no soul. It was a soulless job by the end. And if this thing fails, I don’t know what I’m going to do. I’m going to go be a out-of-hospital midwife somewhere else, because I can’t go back to hospital practice. And maybe that can change. Maybe we can change how we take care of birthing people in the hospital so it doesn’t feel like that midwives have to give up their lifestyle to give holistic care to families.
Jocie: Well thank you. I’m so envious that Neel got to come visit you. I want to see you in action!
Abigail: Come anytime!
Read about how Neel’s visit to Dar a Luz shaped his perspective on anesthesia and movement during labor in his most recent OBservation, originally published in The Conversation
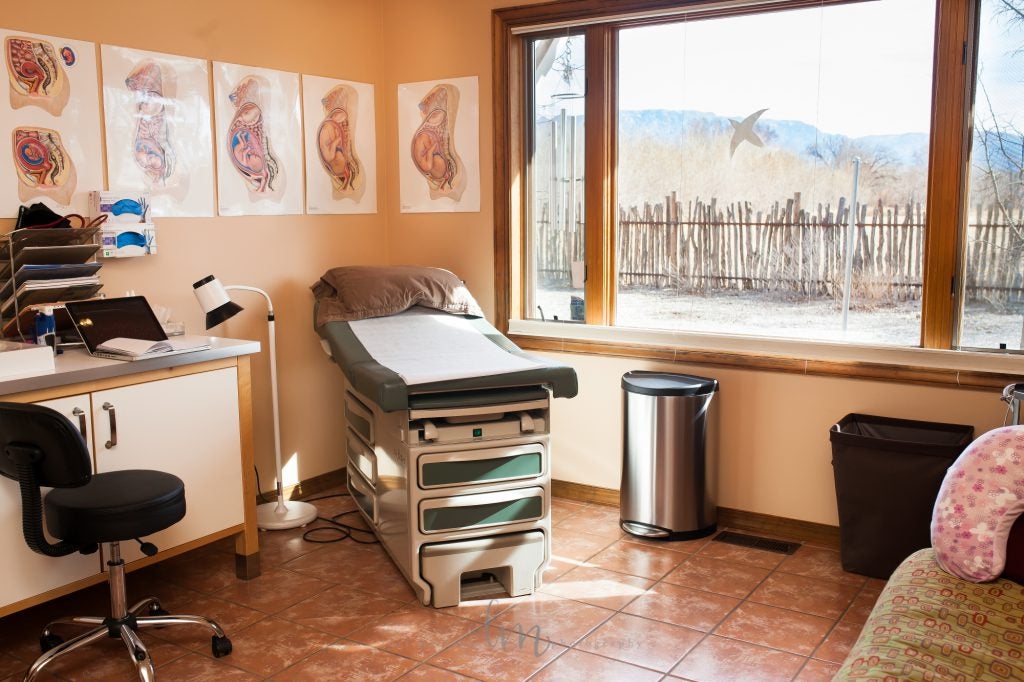
Photography by Lori Martinez
